
Royal College of Obstetricians and Gynaecologists London. National Collaborating Centre for Women’s and Children’s Health. Management of neonatal jaundice in low- and middle-income countries. The Contribution of Neonatal Jaundice to Global Child Mortality: Findings From the GBD 2016 Study. The Neurological Sequelae of Neonatal Hyperbilirubinemia: Definitions, Diagnosis and Treatment of the Kernicterus Spectrum Disorders (KSDs). Le Pichon JB, Riordan SM, Watchko J, Shapiro SM. Long-term neurodevelopmental outcomes after intrauterine and neonatal insults: a systematic review. Mwaniki MK, Atieno M, Lawn JE, Newton CR. Conditions that cause early onset neonatal. Given high levels of pathological jaundice in the first 24 hours and overall high NH burden, guidelines changes were implemented including preventive PT for all neonates <35 weeks and for those 35-37 weeks with risk factors. Jaundice occurring within the first 24 hours of life must be considered to be pathological until proven otherwise. The risk of NH in Sgaw Karen refugees may be overlooked internationally as they are most likely regarded as Burmese in countries of resettlement. The genetic impact of G6PD deficiency on NH was partially interpreted by using the florescent spot test and further genotyping work is in progress. 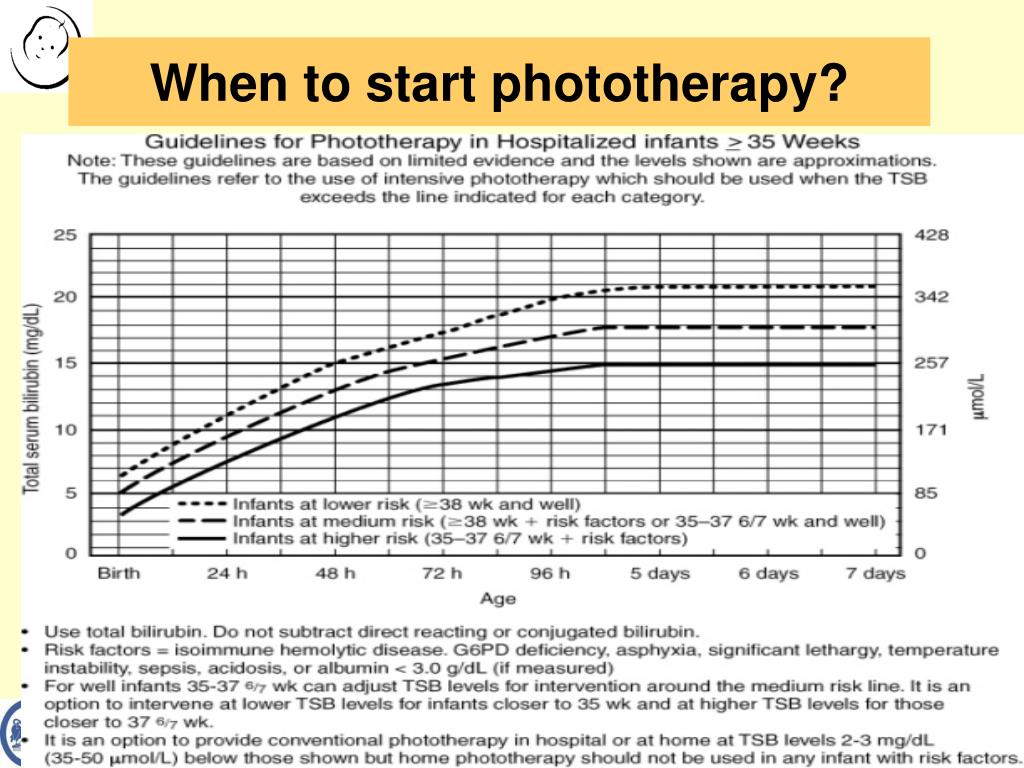
Risk factors for NH in the first week of life independent of gestational age were: neonatal G6PD deficiency, birth bruising, Sgaw Karen ethnicity, primigravidae, pre-eclampsia, and prolonged rupture of membranes. It occurs because of physiological changes taking place during the transition from intrauterine to neonatal life. NH onset varied with gestational age: at a median 24 hours for neonates born 37 weeks or prematurely vs 59 hours for neonates born ≥38 weeks. Pathological Jaundice Physiological jaundice Physiological jaundice occurs in the first few days after birth and will have cleared by day 10. One-quarter (26.3%) of NH occurred within 24 hours. 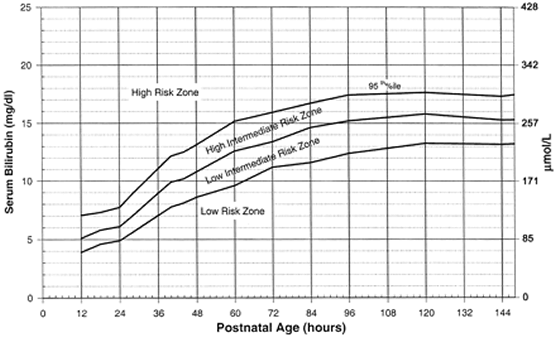
Breastmilk and physiological jaundice are diagnoses of exclusion, only to be. Mortality from acute bilirubin encephalopathy was 10% (2/20) amongst the 5.3% (20/376) who reached the severe NH threshold. Jaundice is pathologic if it occurs in the first 24 hours and requires immediate intervention if the total serum bilirubin level rises by more than 5mg/dL per. Causes that must be urgently ruled out include infections and biliary obstruction. All neonates born <35 weeks, four in five born 35-37 weeks, and three in twenty born ≥38 weeks had NH, giving an overall incidence of 2 livebirths. Risk factors for developing NH were evaluated using Cox proportional hazard mixed model. Each neonate had total serum bilirubin measurements: scheduled (24, 48, 72 and 144 hours of life) and clinically indicated and weekly follow up until 1 month of age. Between January 2015 and May 2016, in a resource-limited setting on the Thailand-Myanmar border, neonates from 28 weeks' gestation were enrolled into a prospective birth cohort. Knowledge of local risks permits interventions that may reduce the proportion becoming severe. Population risks for neonatal hyperbilirubinaemia (NH) vary.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
